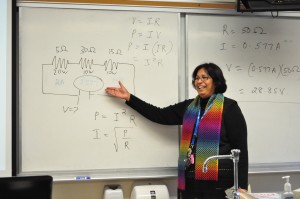
By: Ysé Massot
Photo by: Wendy Qiu
Jacinta Kompella joined the physics faculty on Feb. 3 and is teaching Advanced Placement (AP) Physics B and Physics 1A. Because she came in the middle of the year, Kompella is tasked with the difficult job of covering material that should have been taught during the first semester, as well as continuing the pace of each class.
When the administration began looking for a new physics teacher to replace Eric Hickok, the previous AP Physics B and Physics 1A teacher, they looked for a teacher who was familar with the academic expectations and vigor of Gunn students. “Kompella had been a teacher assistant at Lynbrook High School for six months, and Lynbrook is a similar school to Gunn in type of students,” Instructional Supervisor Eric Ledgerwood wrote in an email. Her familiarity with a competitive learning environment helped Ledgerwood decide that Kompella would adequately prepare AP Physics B students for the AP test and would cover all of the necessary material for each of her classes.
Kompella was also hired based on her strong qualifications, a passion for physics and a strong background in the subject. After graduating from Delhi’s Institute of Technology with a degree in fiber optics, Kompella received a teaching credential from San Jose State University. She then went to work as an engineer for a startup company in the optical communications industry for four years and as an educational consultant for universities such as the University of California, San Diego, Loma Linda University and University of Northern California for seven years.
According to Kompella, she decided to become a teacher for two reasons. First, her last job was very work-intensive, and she believed that teaching would let her spend more time with her children. Moreover, Kompella has always loved teaching. “When I was little, to learn my lessons, I pretended I was the teacher and I taught the lessons to myself,” Kompella said.
According to Kompella, a large challenge she faces this semester is trying to review as much neglected material as possible, while teaching new material thoroughly and in a timely fashion. In order to prepare students for the AP exam at the end of the year, Kompella is working through material faster than some students may have been used to. “Kompella is actively surveying and testing students to see where they are in terms of physics understanding so that she can contour the course and make corrections to her own delivery and style as the year moves forward,” Ledgerwood wrote.
In order to cover double the amount of material in one semester, Kompella is also partnering with other teachers, such as Allyson Frykman, the AP Physics B teacher who went on leave last year. “I continue to teach new topics while going back and firming up on first semester topics to prepare for the AP exam,” Kompella said.
Kompella is also working hard to get to know her students well and tries to make the class as interactive as possible. “Dr. Kompella comes around to check our work and give us some advice personally,” senior Anastasia Petrova said. “She also makes herself very available to us during tutorial or by appointment.”
Kompella’s class places a strong emphasis on developing students’ scientific thinking. “The ultimate and long-term goal is to have a solid understanding of physics and have fun doing it, so that it forms the foundation for their learning in college,” Kompella said.
According to Ledgerwood, Kompella has been managing the class and workload very well. “I believe that Dr. Kompella has been doing great so far,” he wrote. “She has basically made the best of a very difficult situation.”











